Urinary Incontinence
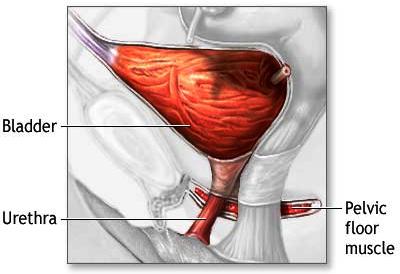
If you have incontinence, this means that you leak urine – in either small or large amounts. Muscles and nerves in and around your bladder work with your brain to store urine and help you empty your bladder when it’s full. If the muscles or nerves aren’t working correctly, this can cause you to have trouble holding your urine or emptying your bladder.
There are two main types of incontinence that are classified based on your symptoms and what’s causing them.
- Urge Incontinence: Bladder leakage that happens in conjunction with a sudden, strong or frequent urge to urinate
- Stress Incontinence: Bladder leakage that occurs when you put pressure on the muscles around your bladder, like when you cough, laugh, sneeze, lift something or exercise
Urinary Incontinence Testing, Management, and Treatment
Urinary Incontinence Testing and Evaluation
Your doctor might perform tests such as:
- Urinalysis: testing a sample of your urine for infection, blood or other abnormalities (read more…)
- Urodynamic Testing: a series of tests to measure how well your bladder and urethra function (read more…)
- Cystoscopy: your urologist looks inside your bladder by inserting a thin tube with a lens in it through your urethra. This helps your doctor check for things like chronic inflammation and bladder stones. (read more…)
Urinary Incontinence Management
You can help prevent urinary incontinence by keeping your bladder healthy with lifestyle changes.
- Avoid food and drinks that seem to increase your symptoms such as caffeine and acidic foods (alcohol, tomatoes, citrus)
- Keep hydrated to avoid your urine getting too concentrated, which can irritate your bladder
- Schedule regular bathroom visits with the goal of gradually increasing the length of time between trips
- Urinate before and after sex and wipe from front to back after a bowel movement to discourage bad bacteria from growing in the urethra and creating an infection
- Eat more fiber and avoid straining during bowel movements. Constipation and straining can put extra pressure on your bladder and weaken your pelvic floor muscles.
- Quit smoking. Persistent coughing from smoking can stress pelvic floor muscles.
- Maintain a healthy weight. Obesity puts extra pressure on your bladder and can make incontinence worse.
Urinary Incontinence Treatment Options
Treatment for bladder leakage depends on the type of incontinence (urge or stress) and its cause. Treatments may include:
- Pelvic Floor Physical Therapy – These help men and women strengthen and control the muscles involved in urination. Kegels are one example of pelvic floor muscle exercises.
- Medicines: If you have urge incontinence, depending on what’s causing it, medicines may be able to help.
- Topical Estrogen (for women): Especially in post-menopausal women topical estrogen can restore the health of the bladder and vagina tissue, allowing them to resume their role in controlling bladder leakage.
- Pessary: This is a small device a provider puts into a woman’s vagina to help support her pelvic muscles and stop leaks.
- Electrical Stimulation and Neuromodulation sends small pulses of electricity to your pelvic muscles to make them tighter and stronger
- Injections of botulinum toxin (BOTOX®) into the bladder muscle to keep it from contracting too often. This treatment wears off and will need to be repeated in 6-9 months
- Surgery and Outpatient Procedures: When other treatments haven’t worked, depending on the type of incontinence and its cause, surgery and outpatient procedures can treat urinary incontinence.
Printable Information
Download our Types of Incontinence educational handout.
Frequently Asked Questions
Is incontinence a normal/expected part of aging?
Loss of bladder control is not normal at any age. It is the sign that there is a problem that you need to discuss with your doctor.
How often should I urinate to maintain good bladder health?
If you are drinking an adequate amount of water (enough that your urine is clear or light yellow), you should urinate every 2-3 hours and wake no more than twice at night to urinate. Holding urine longer can cause it to become concentrated or the bladder to become overfull, both of which increase the likelihood of leaks.













