TURP Surgery (Transurethral Resection of the Prostate)
What is a TURP (Transurethral Resection of the Prostate)?
Transurethral Resection of the Prostate (TURP), is a surgical procedure used to treat urinary symptoms due to BPH (enlarged prostate).
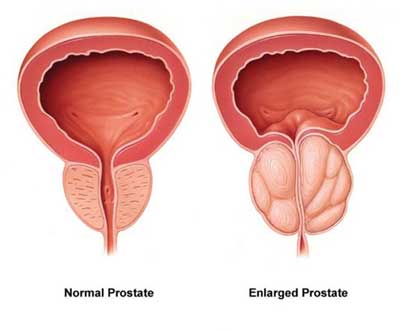
In men, the urethra carries urine from the bladder out through the penis. In men with BPH, the urethra is compressed as due to an enlarged prostate. This can block the flow of urine and cause urinary symptoms like:
- A weak urine stream
- Trouble starting the flow of urine
- Starting and stopping again when urinating
- Not emptying your bladder completely
- Urinating more often, especially at night
- Sudden urges to urinate
- Leaking or dribbling after you urinate
- Straining to urinate
To restore the normal flow of urine, your doctor removes part of the obstructing prostate issue. An anesthesiologist will place you under general anesthesia, which means you will be asleep for the TURP procedure. Occasionally, anesthesiologists may use spinal anesthesia, which means you will remain awake but feel nothing. TURP surgery generally takes about 60 to 90 minutes to complete.
There are no incisions in a TURP procedure. The tissue removal is completed using a thin surgical instrument that travels through the tip of your penis, through the urethra, and into the prostate area.
Potential Side Effects / Risks of TURP Surgery
In addition to the risks associated with any surgery, some of the potential risks of TURP surgery include:
Difficulty Urinating: A temporary problem associated with post-surgery swelling. A catheter may be placed until you’re able to urinate on your own.
Urinary Tract Infection (UTI): After any prostate surgery, there is a risk of a UTI. The longer a catheter is kept in place, the greater likelihood of infection. Some men experience recurring UTIs following TURP surgery.
Retrograde Ejaculation: Also known as dry orgasm, this effect causes semen to travel into the bladder instead of out the penis during ejaculation. While this doesn’t normally affect sexual pleasure and isn’t harmful, it can affect fertility.
Erectile Dysfunction: ED is a rare side effect of TURP surgery, but is possible.
Retreatment: Over time, the prostate may continue to grow and the need for additional treatment may arise. It’s also possible that retreatment may be necessary to treat urethral stricture caused by the TURP.
This is not an exhaustive list of potential risks associated with TURP surgery. Talk to your doctor about all risks and complications prior to surgery.
Before Your Surgery
Three to four days after meeting with your urologist to discuss your surgery, you can expect a call from your surgery coordinator to arrange a surgery date and explain the pre-surgery instructions.
Your urologist is authorized to perform surgery at most major private hospitals in the city. Your surgery coordinator will tell you which hospital or ambulatory surgery center is recommended for your case. You can take comfort in knowing that the staff is used to working closely with your doctor and has the necessary surgical equipment for your procedure.
Medications before surgery
All patients preparing for surgery must stop taking aspirin-containing medications and herbal supplements at least 7 days prior to surgery. These medications interfere with blood clotting and continuing to take them could lead to excessive bleeding during and after your procedure.
If you are diabetic and taking insulin or an oral diabetes medication, do not take your medication the morning of your surgery. The nurse at the hospital will check your blood sugar and give you any medication that may be required.
Eating Before Surgery
Eat a light dinner the evening before your surgery. After midnight, do not eat or drink anything (not even gum, mints or water) unless you have been told otherwise by your surgery coordinator.
Arriving at the hospital
Arrive at the hospital at the time your surgery coordinator has specified (usually 2 hours before your procedure) and report to the “admitting” area for check in.
TURP Recovery
Most patients stay in the hospital 1-2 days following TURP surgery.
Despite the fact that no skin incisions were used, the prostate is quite raw. The prostate has a scab over the area that was treated. Certain precautions are needed to ensure that this scab is not disturbed over the next few weeks while the healing takes place.
Because of the raw surface around your prostate and the irritating effects of urine, you may expect frequency of urination and/or urgency (a stronger desire to urinate). You may also find that you need to get up more often at night to urinate. These symptoms will usually resolve or improve slowly over several weeks.
You may see some blood in your urine over the first 6 weeks. Do not be alarmed, even if the urine was clear for a while and then becomes bloody. If you see blood in the urine, limit strenuous activity and be sure to drink a lot of fluids.
Some patients are sent home with a catheter in their bladder. It is normal to see blood in the urine as long as you have a catheter in place, and you may continue to see blood in the urine for several days after the catheter is removed.
It is important to drink a lot of fluids.
If you are discharged with a catheter in the bladder, your doctor will tell you when to return to the clinic to have the catheter removed. Review our catheter care instructions for more information.
Diet
You may return to your normal diet immediately. Because of the raw prostate, alcohol, spicy foods, and drinks with caffeine may cause some irritation or frequency and should be used in moderation. To keep your urine flowing freely and to avoid constipation, drink plenty of fluids during the day (8-10 glasses).
Activities
Restrict your physical activities for at least the first 2 weeks of recovery. During this time, use the following guidelines.
- No lifting heavy objects (greater than 10 lbs)
- No long car rides
- No strenuous exercise (minimize stair climbing)
- No sexual intercourse until approved by your doctor
Bowel Care
It is important to keep your bowels regular during the post-operative period. The rectum and the prostate are located next to each other in your body, and large and hard stools that require straining to pass can cause bleeding. You may be given stool softeners to prevent constipation. If needed you may take an over-the-counter laxative such as milk of magnesia or Dulcolax.
Medication
You should resume all of your pre-surgery medication unless your doctor tells you otherwise. In addition, your doctor will often provide a stool softener and an antibiotic to prevent infection. You should take the antibiotic as prescribed until the bottle is finished unless you experience problematic side effects. If you experience problematic side effects, call you urologist.
Call your urologist if you experience these problems
- Fevers over 101.5° F
- Heavy bleeding or clots (see section above about blood in urine)
- Inability to urinate









